Hospitals across the country continue to raise concerns about their struggles to stay afloat. A forum Monday night, "Hospitals in Critical Condition," a Fluence Forum with Blois Olson on WCCO Radio will focus on struggles felt by the country's health systems.
Hundreds of rural hospitals across the country are facing closures after years of funding problems, but that struggle is also being felt by hospitals in the core of the largest U.S. cities as well.
That is highlighted by the fight for Hennepin County Medical Center to stay afloat in Minneapolis. That system is facing closure unless state funding is granted through the Minnesota Legislature.
HCMC is the state's premier level one trauma center, that treated patients following last year's Annunciation Church shooting, and is frequently the first stop for the most dire of emergency situations in the state.
The head of the hospital board, Hennepin County Commissioner Jeffrey Lunde, says they were able to find $50 million dollars in cuts in order to survive the first quarter of the year - but they still have to find $125 million more to cut by the end of the year, a massive number they say isn't survivable.
"We just want to be clear to everyone that the situation at HCMC is dire," Lunde says.
The issue was compounded last summer by the Trump administration’s massive cuts to Medicaid, the government’s safety net for low-income Americans, whose reimbursements have long helped hospitals meet their bottom lines.
One of the experts joining the forums is United Hospital District CEO Rick Ash, who tells the WCCO Morning News with Vineeta Sawkar that OBGYN and delivery programs in rural Minnesota have been hit especially hard.
"About 11 years ago when I first got here, we had OB in every county around us," says Ash. "Today, 19 programs across Minnesota have closed, and patients are driving 60-plus miles to give birth. And not to get into too much detail, but we've had a couple of occurrences where it's been nip-and-tuck for babies. Fortunately we were here."
Outcry over the funding cuts prompted Republican lawmakers to create $50 billion in new rural health grants, but critics say that funding is intended for innovative health care delivery solutions — not propping up hospitals buckling under current pressures.
“It won’t pay to keep the lights on. And it won’t turn the lights back on once they’ve been turned off,” said Dr. Ben Young, an infectious disease specialist and policy expert with public health advocacy group Wellness Equity Alliance.
Administrators say the new $50 billion fund is not meant to shore up ailing rural hospitals or maintain the status quo, but to transform rural health care through tech, workforce and other innovations. Centers for Medicare and Medicaid Services Administrator Dr. Mehmet Oz in a December video said it “gives states the tools to design solutions that last, not Band-Aids that fail.”
However, Ash says the crisis is becoming so widespread, he believes every hospital in the state is feeling the financial strain, with a shocking admission of significant loss coming off as a positive in his eyes.
"We are fortunate that we've been doing fairly well," Ash says of United Hospital, where he works. "We've only lost $1 million so far this year, and we've been able to find ways to cover that. But it's going to continue to get worse. I know hospitals colleagues that are trying to make payroll, trying to get short-term financing just to make payroll."
Cuts to Medicaid funding vary by state. In Minnesota, the state is looking at a 15% cut, which amounts to approximately $19 billion over the next decade, and that's money hospital systems can't come close to making up.
As for that $50 billion coming from the Trump administration to rural hospitals? It amounts to just over $193 million.
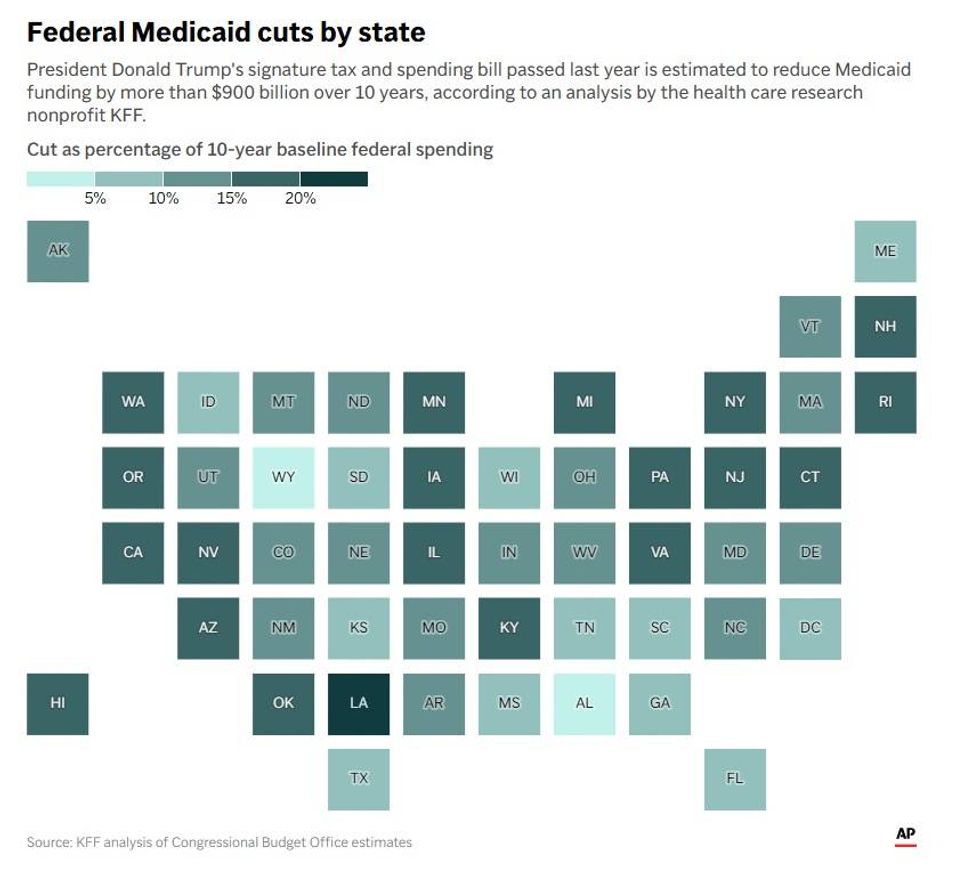
President Donald Trump's signature tax and spending bill passed last year is estimated to reduce Medicaid funding by more than $900 billion over 10 years, according to an analysis by the health care research nonprofit KFF.
(Associated Press)
Significant number of hospitals across the country facing financial distress
Minnesota hospitals, and many across the U.S., are facing a severe financial and operational crisis.
Nearly 25% of the hospitals in Minnesota are in financial distress, with many, including major urban safety net facilities like Hennepin Healthcare, at risk of closing.
But why? What's happened?
There are a number of factors at work like those federal funding cuts, which will eventually slash billions of dollars in health care funding.
Also, government programs like Medicaid often don't reimburse hospitals at the same cost of the care. This is compounded by a growing number of uninsured patients or even underinsured patients, leaving hospitals with huge amounts of debt and uncompensated care.
It’s also costing more to operate a hospital. Inflation is driving up the cost of supplies, services, faculty maintenance, and the cost of labor with widespread staff burnout since the COVID-19 pandemic.
Jan Malcolm, the former Minnesota Health Commissioner, and now senior adviser to Minnesota Governor Tim Walz on hospitals and health care systems, testified before lawmakers recently about the crisis and what's making it worse.
"Like the closure of UCare, the national change healthcare claims payment system debacle and the impact on patient care from the metro surge,” says Malcolm.
And it's not just about money.
“Our health system leaders are saying that the business model of healthcare - the business model of healthcare - is fundamentally broken,” Malcolm added.
So what's next in the short term, in the long term, and can Hennepin Healthcare survive in this new world of healthcare funding?
Malcolm says look to Hennepin County Medical Center for guidance, because that, she says, is just the start.
“The trends are also beginning to affect other hospitals around the state,” she adds.
Multiple proposals to bolster HCMC’s finances have been discussed this legislative session, with three of the committee’s members presenting their own proposals recently. All of this highlights the issues facing every state across the U.S. - how do we make up the gap of lost federal funding?
- HF4841, sponsored by Rep. Esther Agbaje (DFL-Mpls), would increase a 2007 Hennepin County sales tax used to fund construction of Target Field from 0.15% to 1% and allow revenue from the tax to also go toward county healthcare facilities like HCMC;
- HF4892, sponsored by Rep. John Huot (DFL-Rosemount), would temporarily use the state’s General Fund surplus to help cushion HCMC while the hospital and state work to resolve funding issues; and
- Rep. Danny Nadeau (R-Rogers) presented a yet-to-be-numbered bill that would dedicate $250 million from the General Fund each year to go to HCMC and North Memorial Hospital. After five years, the amount to HCMC would decrease as the hospital is expected to work toward cost efficiency. The bill would also require the governance of the Hennepin County Hospital Board to transition to 80% membership with professional education and experience working in health system and safety net hospitals.
Rural areas losing healthcare at staggering rates
As many as 140,000 Minnesota residents will lose their health coverage due to federal Medicaid cuts rolling out over the next few years. That's according to an analysis by the Minnesota Department of Human Services, and state Medicaid director John Connally says unfortunately rural hospitals are in the bullseye.
“Often in many communities in Greater Minnesota or rural parts of Minnesota, there is a higher share of people in the community who rely on Medicaid for their health coverage, and therefore the hospitals in those communities rely more disproportionately on Medicaid relative to some facilities in the metro areas.”
Officials with the Minnesota Hospital Association say more than 30 hospitals in the state are in financial distress right now, and Dr. Rahul Koranne is the association's president and CEO.
“I'm very afraid that some of these hospitals will be forced to close, and who is going to lose? It's going to be Minnesotans and Minnesota families,” Koranne says.
But despite some of the grim predictions over the future of rural healthcare, a gleaming new University of Minnesota Medical school campus in St. Cloud is training its first class of 24 new rural doctors.
“This can be set up like a hospital bay, a trauma bay,” says Dr. Jill Amesbury who is the Medical School's assistant dean, tasked with addressing a serious shortage of rural physicians in Minnesota.
She's an optimist who says two things can be true: yes, there can be some real challenges in how we deliver healthcare in a rural setting, such as the cuts to Medicaid, and she says we can have great hope.
“What we can't do is nothing,” she says. “We cannot sit back and just watch our rural health systems close.”
Rural health fund billed as a cure falls short
The $50 billion Rural Health Transformation Program included in President Donald Trump’s tax-and-spending law last year was billed by Republicans as a way to help hospitals in rural areas. Last summer, Health Secretary Robert F. Kennedy Jr. touted it as the “biggest infusion in history” for rural hospitals and pledged it will “restore and revitalize these communities.”
Hospitals and health industry experts have warned that while the fund — $10 billion per year allocated across all states for five years — offers some support to struggling rural hospitals, it won’t save them. One reason is that the sum doesn’t come close to offsetting the $137 billion that rural hospitals expect to lose over the next decade, according to health research nonprofit KFF. Millions of people are expected to lose Medicaid benefits as a result of new Medicaid work requirements going into effect in 2027 — changes the Trump administration has maintained will crack down on fraudsters rather than cut off eligible enrollees.
Administrators say the new $50 billion fund is not meant to shore up ailing rural hospitals or maintain the status quo, but to transform rural health care through tech, workforce and other innovations. Centers for Medicare and Medicaid Services Administrator Dr. Mehmet Oz in a December video said it “gives states the tools to design solutions that last, not Band-Aids that fail.”
The White House echoed that, saying the fund is intended to fund “big ideas” to improve rural health care access long-term.
“Decades of mismanagement by career politicians in Washington have left rural communities with limited care options,” White House spokesman Kush Desai said.
State applications show a wide range of proposals. Some pitches sought to improve emergency medical services and modernize rural facilities, while others looked to make school lunches healthier, expand physical fitness programs, beef up telehealth and expand AI-driven technologies to help monitor patients.
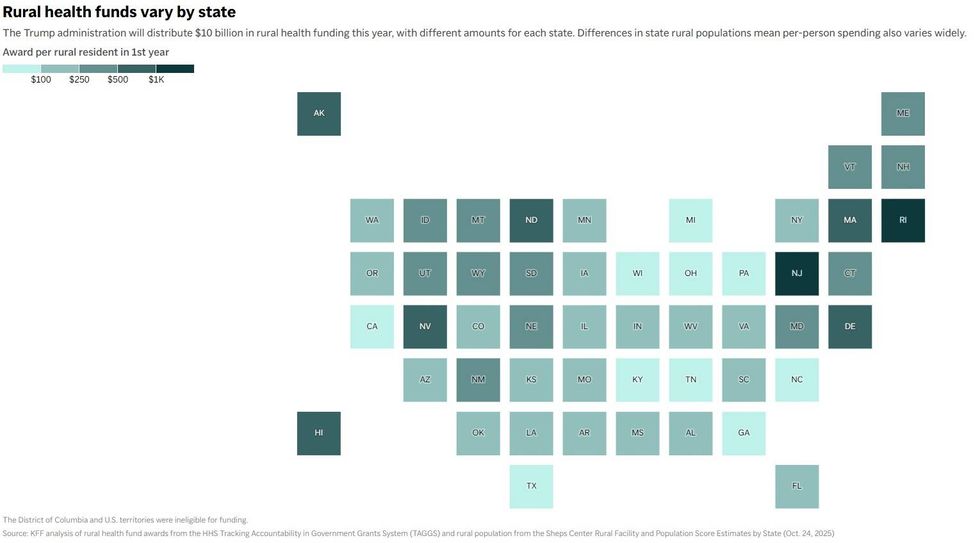
The Trump administration will distribute $10 billion in rural health funding this year, with different amounts for each state. Differences in state rural populations mean per-person spending also varies widely.
(Associated Press)
Hospitals in Critical Condition Forum:
5:00-5:30 p.m.
Rahul Koranne, CEO MN Hospital Association and Jan Malcolm, and Fmr. Commissioner MN Dept of Health
5:30-6:00 p.m.
Dr. John Cumming, CEO of Hennepin Healthcare, Rick Ash, CEO of United Hospital District (Blue Earth), and Rick Breurer, CEO, Community Memorial Hospital
6:00-6:30 p.m.
Rachelle Schultz, CEO - Winona Health, Greg Ruberg, President - Aspirus Lake View Hospital (Two Harbors), and James Hereford, CEO - Fairview Health System
6:30-7:00 p.m.
Sen. Paul Utke (R- Park Rapids), and Rep. Robert Bierman (DFL – Northfield)
A WCCO Radio, Fluence Forum, explores the state of healthcare in the face of significant financial worries for hospitals and patients
A WCCO Radio, Fluence Forum, explores the state of healthcare in the face of significant financial worries for hospitals and patients








